Ivy Blog
What is an Awake Craniotomy?
- December 21, 2022
- Ivy Center
- Posted in Glioblastoma
By Sarah Key, MS, CCC-SLP, Ivy Brain Tumor Center at Barrow Neurological Institute
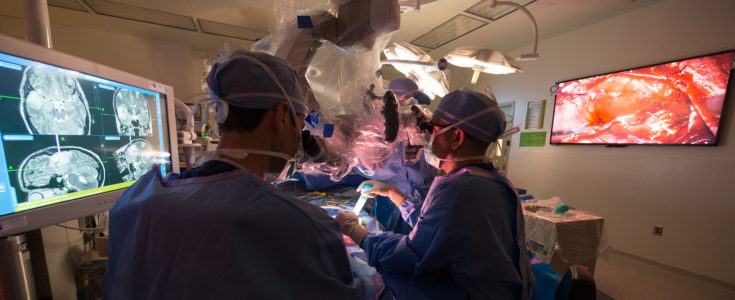
Brain surgery performed while the patient is awake is called an awake craniotomy. This technique allows neurosurgeons to maneuver around eloquent areas of the brain while safely removing tumor tissue. If the tumor is near parts of the brain that control vision, movement or speech, the surgeon or speech language pathologist will ask the patient questions and monitor activity in their brain as they respond. This can lower the risk of damage to functional areas of the brain.
Neurosurgeons at the Ivy Brain Tumor Center at Barrow Neurological Institute perform more than 100 awake craniotomies annually. Here are some of the most common questions asked by patients.
What is the benefit of an awake craniotomy?
Brain mapping is considered the gold standard for the identification and preservation of critical brain areas, such as those important for language and motor function. When a portion of a brain tumor or lesion is near a critical area, brain mapping allows your neurosurgeon to locate the precise areas of the brain that are important for certain functions and then avoid them during removal of the tumor. With this information, along with detailed brain images, neurosurgeons, such as Nader Sanai, MD, director of the Ivy Center and Neurosurgical Oncology at Barrow Neurological Institute, can resect as much of the tumor as possible while also minimizing the risks of damage to important functions.
What can I do to prepare for awake brain surgery?
You will undergo a series of meetings prior to surgery to guide surgical decision-making. You will speak with a neuroanesthesiologist who will discuss in detail how you will be put to sleep and woken up during surgery, as well as any medical factors that affect anesthesia. During a consultation with a speech language pathologist (SLP), information will be gathered about your current speech and language functions. The SLP will also present certain language tasks that can be used during the mapping procedure in order to make sure you are accurate and familiar with these tasks. Additionally, you will meet with a neuropsychologist who will conduct functional Magnetic Resonance Imaging (fMRI), a type of imaging that detects changes in blood flow and oxygen levels that occur when an area of the brain is activated. During the fMRI scan, you will be asked to complete a variety of simple language and motor tasks while inside the scanner. The resulting fMRI “activation maps” identify areas of the brain that are important for language and motor function. These maps are used to enhance the neurosurgery team’s ability to make informed decisions concerning the surgery and will be available to the surgeon during the operation.
Finally, you will meet with another neuropsychologist to assess your overall cognitive and emotional functioning. This will consist of a brief interview and a few pencil and paper tests. In addition to identifying cognitive strengths and weaknesses that can inform treatment, this assessment will establish a baseline from which any future cognitive or emotional changes can be measured. All of the information gathered by the neuropsychologists, neuroanesthesiologist, and SLP will be communicated directly with the neurosurgeon. Studying pictures or “practicing” for awake mapping is absolutely not necessary. Rest and activities that support relaxation are best in the days leading up to surgery.
What happens during awake craniotomy surgery?
You will be asleep for the first portion of the surgery. Initially, you will move to the operating room table, vital sign monitors will be attached and the anesthesiologist will have you breathe oxygen from a face mask. Next, medication will be given through the IV to put you to sleep. At this point, a device called a Laryngeal Mask Airway (LMA) will be placed in the back of your throat above the windpipe. Then, you will be positioned on your side at a 45-degree angle with one arm out on an armrest and another lying by your side. Your head will be placed in stabilization pins so when you wake up you won’t be able to move your head. You will be under general anesthesia and “asleep” while the neurosurgeon opens the skull (craniotomy) to expose the area of the lesion. Next, the neuroanesthesiologist will lift sedation and remove the LMA. When you are awake, you will be guided through the series of tasks that comprise the brain mapping part of the procedure. Typically our patients are awake for approximately 30 minutes, depending on the location of the lesion and which functions we may need to map. When we have collected all the information that is needed, you will be put back to sleep and the LMA is replaced (or you are intubated with a breathing tube in the windpipe) for the remainder of the surgery.
What should I expect when I wake up during surgery?
When you wake up, you will be lying on your side and your head will be secure. You will see a small tent-like drape over your head and members of the team, including the neuroanesthesiologist and the SLP, orienting you and guiding you each step of the way. We will remind you to remain still and help you stay as comfortable as possible. If you need the temperature adjusted or a slight position change, you can tell us and we will help you. The first thing you will be asked to do is to take slow, deep breaths. Typically it takes several minutes for a patient to wake up fully, so we will give you the time you need to become alert enough to participate in mapping.
When you are fully awake, we will present a series of tasks, such as having you count or name pictures on an iPad to assess language. You will be familiar with these specific tasks because they will be the same tasks you completed when you met with the SLP before surgery. As you do these simple tasks, the neurosurgeon will provide electrical stimulation to areas of the brain to see if the stimulation affects your neurological function. It is important to remember there are no right or wrong answers. For example, electrical stimulation may cause your arm to contract or make you temporarily stop speaking. This response is exactly how we are able to identify a precise area of function.
Will I feel any pain during awake brain surgery?
Brain tissue actually does not have pain receptors and your scalp will be fully anesthetized, so while you may feel pressure or vibrations, you will not feel pain during the operation. If you do feel discomfort, please let the team know and we will do everything we can to alleviate it.
What happens after surgery?
After the surgery is complete, you will move to a post-surgery recovery unit and then to a room in our Neuro ICU for close monitoring for about 24 hours. While admitted in the hospital, you will be seen by multiple disciplines, including your neurosurgical residents, neurosurgical nurse practitioners, and a neuro-oncologist. Additionally, a team of therapists (physical therapy, occupational therapy, speech therapy) will evaluate your physical functioning, abilities to conduct activities of daily living and your language production. The therapists will determine if you may need additional therapy during or after the hospitalization. Typically, patients stay in the hospital for two to four days before going home with outpatient therapies or to an acute inpatient rehabilitation center.
Despite the benefits of awake language mapping, it is usual for a patient to experience increased difficulties with speech and language postoperatively, which are associated with the effects of postoperative swelling within the first days. Usually, these deficits will subside and language will improve with time as postoperative swelling decreases. Evidence indicates this “transient aphasia” is very common after resective surgery and nearly all language deficits resolve by one-month post-surgery. Your speech language pathologist will work with you following surgery to evaluate your language and determine what types of therapy interventions may be indicated to help you. You may also be asked to return for a follow-up neuropsychological assessment a few months after your surgery.
If you are interested in seeking a second opinion from a neurosurgeon at Barrow Neurological Institute, please visit Barrow Second Opinion.
Our mission at the Ivy Brain Tumor Center is to increase life expectancy and contribute to a cure for malignant brain tumors by pioneering the world’s largest, most advanced Phase 0 clinical trials program. For more information, click here or call 602-406-8605.
Medically reviewed by Nader Sanai, MD, Director of the Ivy Brain Tumor Center and Director of Neurosurgical Oncology at Barrow Neurological Institute